“Deme Bones” – inter-limb deviation related to the musculoskeletal pain syndromes
“The toe bone is connected to the foot bone” is the common reframe from the old gospel song “Dem Bones.”
The concept of mechanical connectedness or regional interdependence applied to musculoskeletal pain syndromes suggests that in addition to examining a patient’s local area of complaint examination of the adjacent joints above and below the primary joint should occur.
In this blog, I make the argument that examining the opposite side of the body from the side of the body of the painful joint can lead to interesting conclusions.
What happens when the right rear tire of a car is low on pressure compared to the pressure in the left rear tire?

bent wheel disc
Pain in the right foot results in a limp. A limp is spending less time on the right painful side and more time on the left uninjured side. Impaired movement on one side can make up for or compensate for it with altered movement on the other side.
At times the compensatory movement is more subtle than an obvious limp. There may not be an obvious limp, but a subtle asymmetry of movements. Inter-limb asymmetries of movement and function are comparing the movement of one limb with respect to the other. The assumption is that walking and running movements on the right side of the body should match the left-side movements.
What happens when there is greater force or pressure on one side of a wheel or balloon?

There is evidence that relatively small asymmetrical movements on the order of 5% to 15% difference are common in normal healthy walking and running. Leg dominance, laterality preference such as preferred and skill movement naturally occurs on one side much like being “right-handed.”
The question arises when do asymmetrical movements or inter-limb asymmetries of movement become problematic.
Are there particular gait deviations that typically are associated with inter-limb asymmetries?
Walking versus running mechanics
Inter-limb asymmetries of movement are more likely to manifest in running as compared to walking.
When walking there is always one foot in contact with the ground. When running there is a period when no foot is in contact with the ground. The magnitude of forces walking occurs on both sides of the body during the period of double support. The magnitude of involved forces is greater in running.
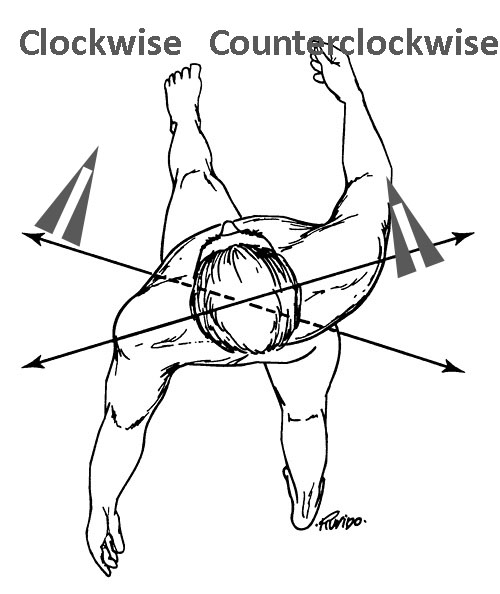
Another difference when walking is the thorax and pelvis move in the same direction. However, when running or walking fast the thorax and pelvis move in opposite directions. While the thorax is moving in a counterclockwise direction the pelvis moves in a clockwise direction.
Running requires propelling the body up and forward. This occurs primarily via the action of the calf, hamstring, and thigh muscles. If one of these muscles is weak on one side of the body to avoid drifting to one side of the road some other region of the body needs to compensate. The muscles which compensate can be on the other side of the body.
What happens when the right rear tire of a car is accelerating faster than the left rear tire? This is analogous to always running counterclockwise on a track.
Inter-limb gait deviations
In my experience, there are three gait deviations that raise suspicion of a potential inter-limb deviation related to the musculoskeletal pain syndrome, they are:
- Asymmetrical arm swing/trunk rotation: The arm bone is connected to the thorax bone, and the leg bone is connected to the pelvic bone. Therefore, when we observe an asymmetrical arm swing there is asymmetrical movement of the thorax. When we see one arm moving farther across the midline of the body more than the opposite arm it is likely the thorax is rotating more in one clockwise or counterclockwise direction.
- Foot crossing the mid-line of the body: When viewed from behind/front at foot strike the opposite foot is not visible; a vertical line from the sacrum or belly button to the ground during stance touches the inside of the heel.
- Asymmetrical toe out (foot progression angle): When viewed from the front or behind the position of the foot relative to the line of progression is more than 5° to 10°; when viewed from behind more than two of the lateral toes are visible.
Examples patient cases
Right buttock pain left knee pain: A fifty-something female and an avid fitness enthusiast performing calisthenics and power walking complained of right buttock pain. An MRI showed a tear of the gluteus Medius tendon and an old tear of the right hamstring.
Previous medical history she reports there is a botched right foot surgery to correct a bunion.
Slow motion video gait analysis of her power walking there showed asymmetrical arm swing, right foot crossing the mid-line of the body, and increased toe out during the stance phase on the right.
During her rehab for the right buttock pain left knee pain occurred.
In addition to providing traditional remedial exercises for gluteal tendinopathy cues, prompts, and feedback described in this blog post are appropriate interventions.
Chronic recurring left hamstring and Achilles injury: Experienced a female marathon runner with recurring Achilles and hamstring injuries on the left side. Long-standing history of hallux valgus (large bunion) on the right foot. There are visibly smaller and weaker right calf and hamstring muscles. The habitual gait pattern showed asymmetrical arm swing, asymmetrical trunk rotation, right foot crossing the mid-line of the body, and increased out-toeing on the right during the stance phase.
Intervention focusing on the dysfunctional gait was successfully applied.
Chronic side stitch: Ultramarathon runner with a complaint of the right-side stitch. Slow motion video analysis revealed asymmetrical arm swing, asymmetrical trunk rotation, and right foot crossing the midline of the body.
Previous medical history included a left ankle fracture.
This blog article describes the cueing, prompting, and feedback processes to alter the old habitual asymmetrical gait deviation.
The above case studies provide examples of how impairment on one side of the body may be addressed by observing asymmetrical gait and intervening to alter the asymmetrical gait.
Like car tire asymmetries significantly increase the risk of a tire blowout, inter-limb movement asymmetries can be related to musculoskeletal pain syndromes.
A on demand-video webinar exploring this topic is available at Plus by Physiopedia entitled “Gait deviations associated with pelvis & knee pain syndromes”
Use this code – “Damien30” for a 30% discount to access this webinar as well as the more than 500 continuing education webinar courses available at Plus by Physiopedia. This is the link http://bit.ly/DAMIEN30 with the 30% discount code embedded.
The information on this website is not intended or implied to be a substitute for professional medical advice, diagnosis, or treatment. You are encouraged to perform additional research regarding any information contained available through this website with other sources and consult with your physician.
Damien Howell Physical Therapy – 804-647-9499 – Fax: 866-879-8591 At-Home, At Office, At Fitness Facility – I come to you, I do home visits Damien@damienhowellpt.com